Modern healthcare
is expensive, especially surgery performed in a regular operating theatre.
General anesthesia involves life-threatening risks and undesirable
side-effects. Local anesthesia minimizes these drawbacks and can be
administered by the surgeon. This promotes simplification.
FREE FULL TEXT Ref: Camera trocar lifting in office gasless laparoscopic sterilization under local anesthesia. Bergström Bo S. Acta Obstetricia et Gynecologica Scandinavica, July 2010, Vol. 89, No. 7, Pages 975-979.
• Room air, two strings and a needle instead
of a CO2 gas filling machine and narcosis.
• Local anesthesia and mild sedation.
• Walking to and from the operating room.
Laparoscopy by using an amnioscope
- sterilization without narcosis - sterilisering utan narkos
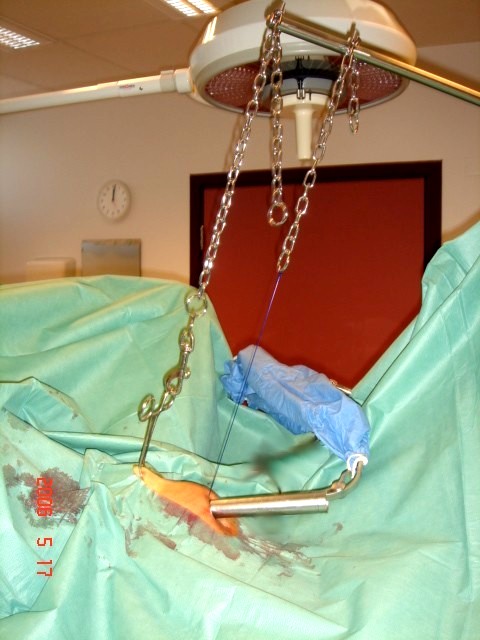
Lifting technique
An ordinary anesthesia frame with the horizontal
arm draped in a sterile sleeve, can be used
 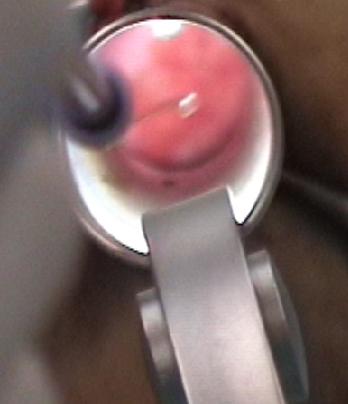
Amnioscope (20×200×25 mm). Direct visual inspection and instrumentation.
Short laparoscopic instruments are used for an optimal visual distance. (Video)
or
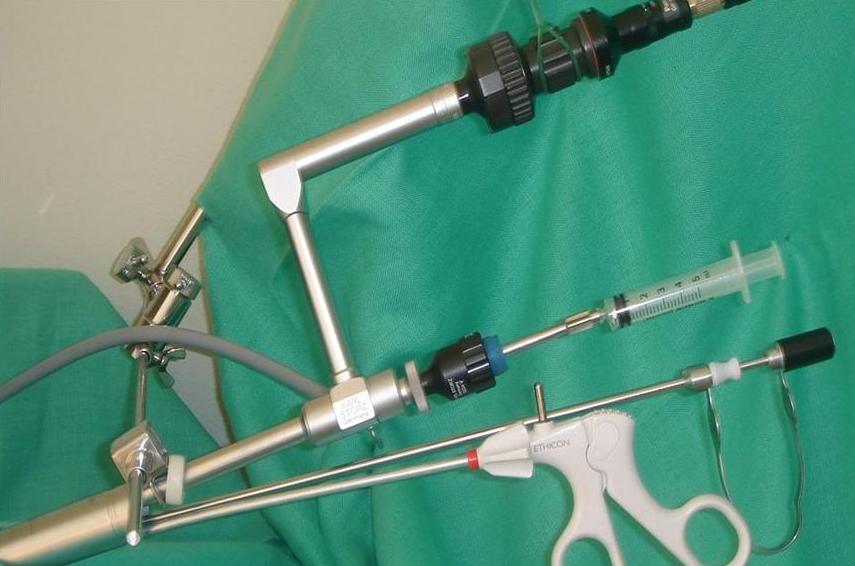  
Amnioscope + Laparoscope. Supports a high inflow of room air and to insert a second working instrument beside the laparoscope to displace obscuring loops of distended bowel, if any.
or
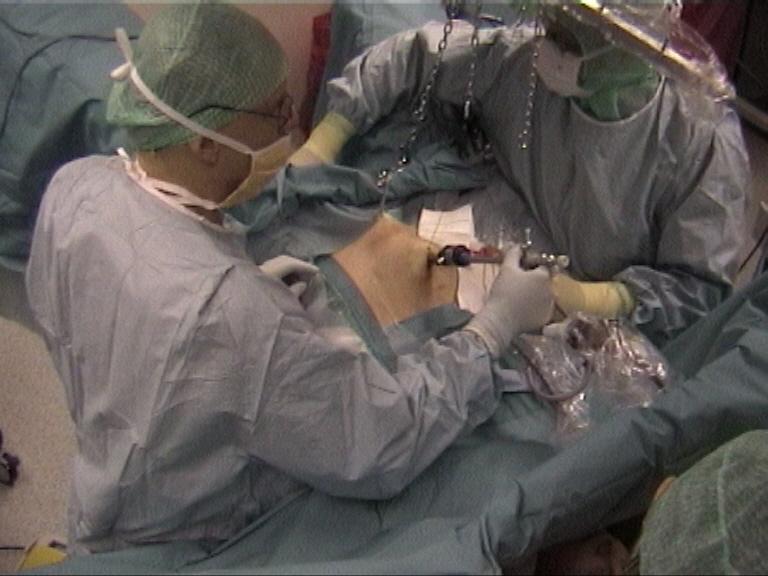 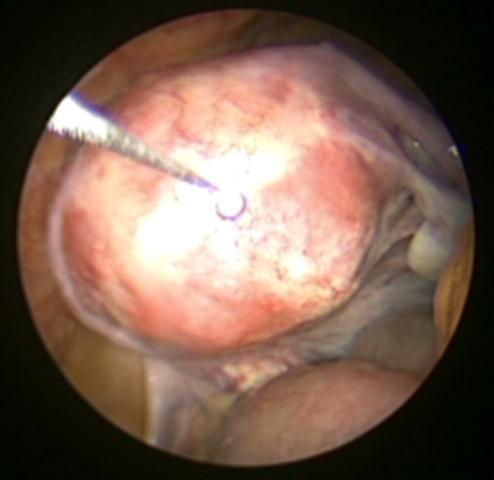
Conventional camera trocar (≥ 12.5 mm with an open high-flow gas inlet) + Laparoscope (≤10 mm) (Video)
--------------------------------------------------------------------------------
An open access technique for trocar insertion is safer than a closed access technique and is therefore a better choice for office laparoscopy. The open access technique results in a 1.5-2 cm wide hole in the abdominal wall so using a micro-laparoscope is meaningless. An ordinary laparoscope has advantages in focal distance and field of vision.
The abdominal wall just beneath the umbilicus and the skin/subcutaneous tissue 6–8 cm above the symphysis pubis are anesthetized (a needle). An amnioscope (or a conventional camera trocar) is inserted using an open access technique. The amnioscope/abdominal wall complex is lifted with a strong loop suture - e.g. PDS#1 (string 1), snared around the amnioscope with a hang knot and needle-driven through the fascia, subcutaneous tissue and skin in the lower end of the abdominal wall incision. The loop suture is attached to a horizontal metal arm mounted on the operating table and placed above the patient (e.g. an anesthesia frame with the horizontal arm draped in a sterile sleeve). The skin and the subcutaneous tissue above the symphysis pubis are lifted in the same way using a towel clamp (string 2). The combination of mechanical lifting, passive intra-abdominal room air filling, Trendelenburg position and forward rotation of the uterus (Hulka forceps) creates adequate intra-abdominal space for inspection and instrumentation. Padded shoulder supports are an important prerequisite.
The woman walks to and from the operating room. She is awake, has full control over her body, is continuously informed by the surgeon and leaves for home after few hours of rest.
Office gasless laparoscopic sterilization requires no scheduling of surgery according to the woman’s menstrual cycle, has an almost 100% first attempt success rate, an immediate effect on fertility, no need for tubal patency control, no material costs and a reversal success rate of 55–75%, an unchanged possibility of IVF and can be performed within 48 hours of delivery.
A comparative study - literature review - of laparoscopic tubal sterilization versus hysteroscopic sterilization showed an overall standard complication rate for laparoscopic sterilization of 0.8 - 0.9% and a major complication rate for hysteroscopic sterilization of 3.2%. Moreover, correct use of local anesthesia removes the single greatest source of risk in conventional laparoscopic sterilization procedures - general anesthesia.
Office laparoscopy
is claimed to cost much less than traditional laparoscopy. In one study, there
was an almost 80% reduction in costs,
which is in agreement with the present study. Our total costs in 2006 were
calculated to be NOK 2,895 (US $446), which represents a 75% reduction. Gasless laparoscopic sterilization and Essure hysteroscopic sterilization can both be performed in an office-based setting with the same OR-team and operation time. The Essure procedure is however approximately US $1600 more expensive due to additional costs for Essure devices (Essure® ESS305 Company: Conceptus, Inc. Retail Price: $1299) and for tubal occlusion control (HSG US $300). Essure hysterosopic steilization is contraindicated within 6 weeks after delivery and to women with hypersensitivity to nickel or allergy to contrast media.
Serious systemic illnesses are indications rather than contraindications for gasless laparoscopy under local anesthesia, but women with such illnesses are not usually operated on in an office-based setting.
Room air, two strings and a needle, replace a CO2 gas filling machine and narcosis.
Office sterilization
Simplicity & Quality
|